Scar Revision Treatment in Mumbai: Smooth, Confident Skin with Expert Care
What Is Scar Revision Surgery?
Scar revision surgery is a cosmetic or reconstructive procedure designed to improve the appearance of a scar or restore function to an area affected by scarring. The goal is to make the scar less noticeable by blending it with the surrounding skin in tone and texture. It can also address discomfort, tightness, or restricted movement caused by thick or deep scars.
Scar revision may involve surgical excision, skin grafting, laser therapy, dermabrasion, or injectable treatments, depending on the type, location, and severity of the scar.
Synonyms of Scar Revision Surgery:
Scar improvement surgery, Scar correction procedure, Scar removal surgery, Scar refinement treatment, Scar remodeling surgery, Scar concealment procedure, Keloid or hypertrophic scar revision, Cosmetic scar correction, Reconstructive scar surgery, Laser scar revision, Post-surgical scar correction, Trauma scar improvement
“Ready to reshape your body?”
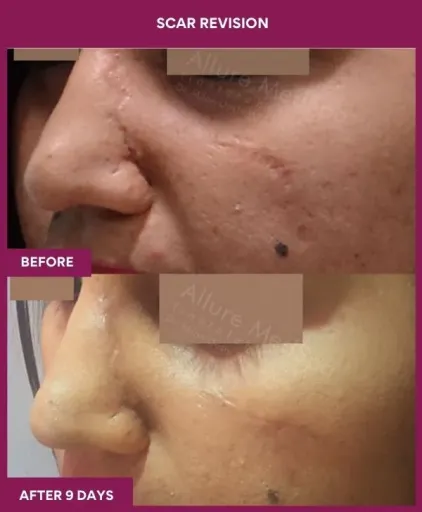
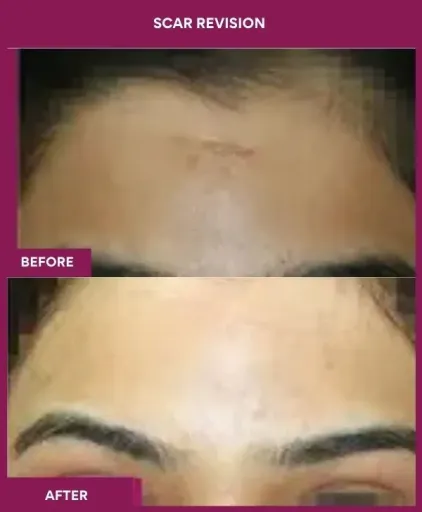
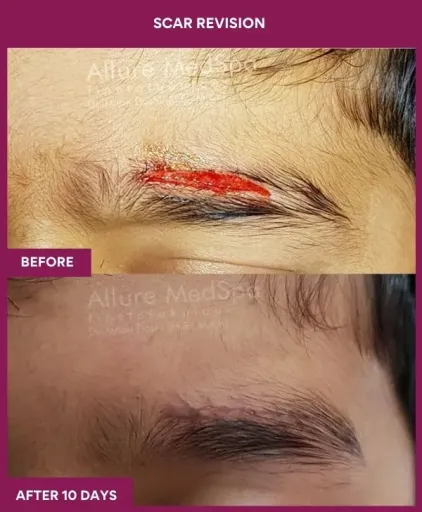
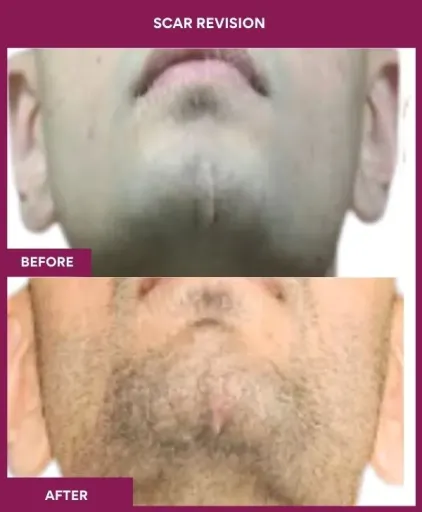
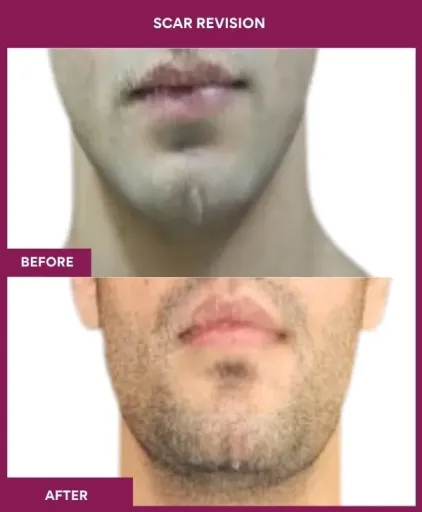
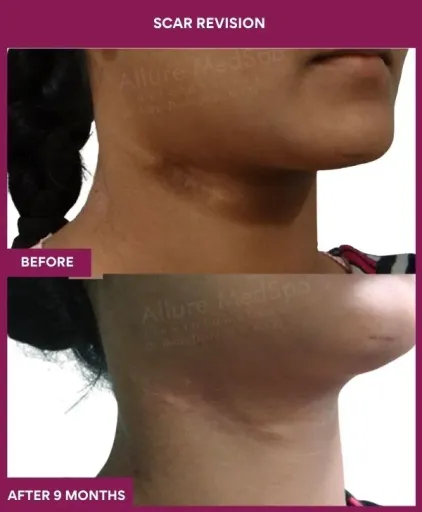
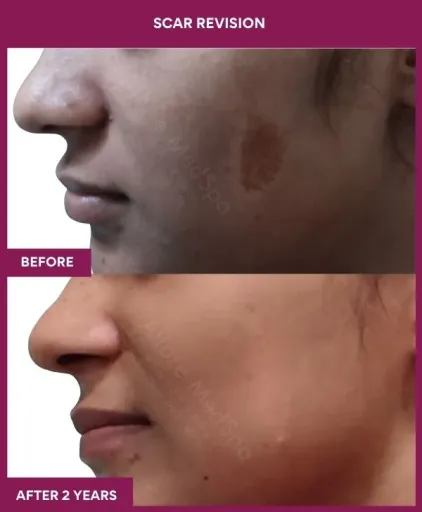
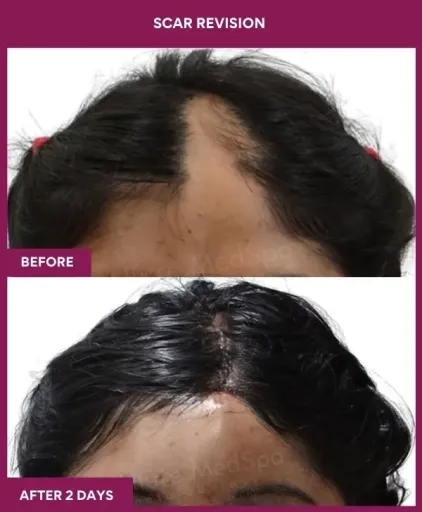
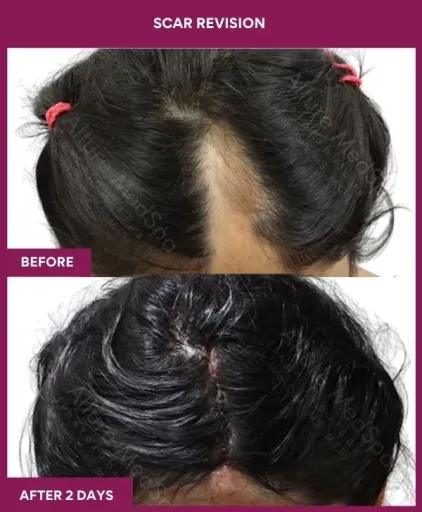
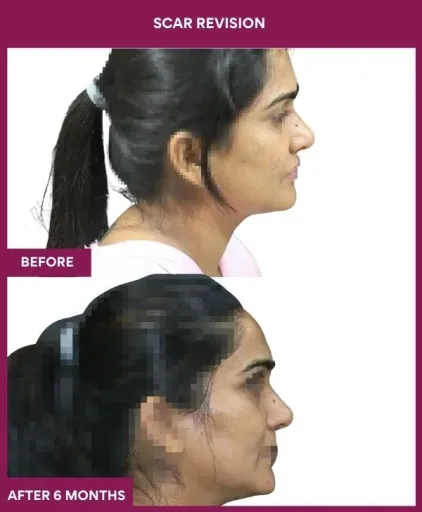
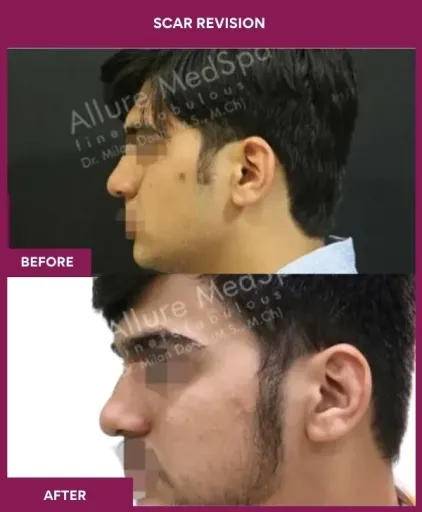
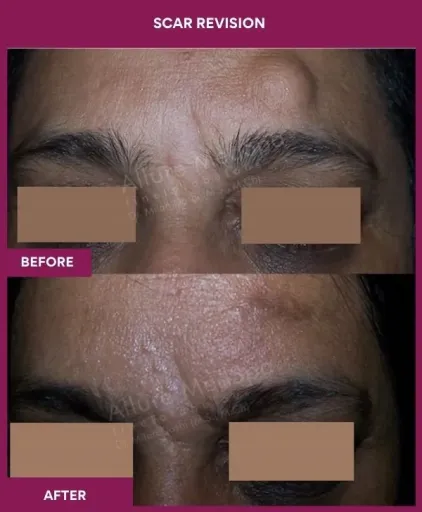
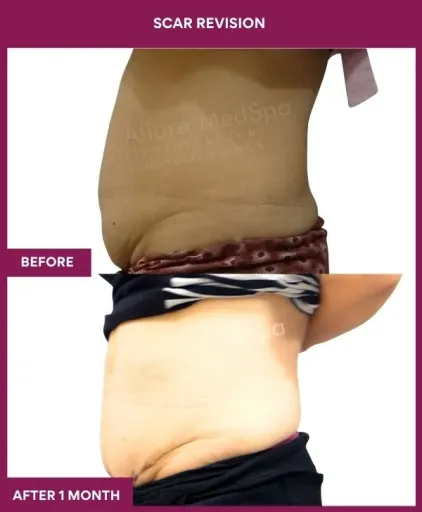
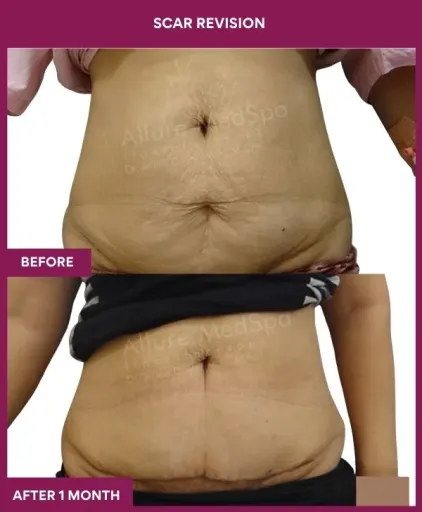
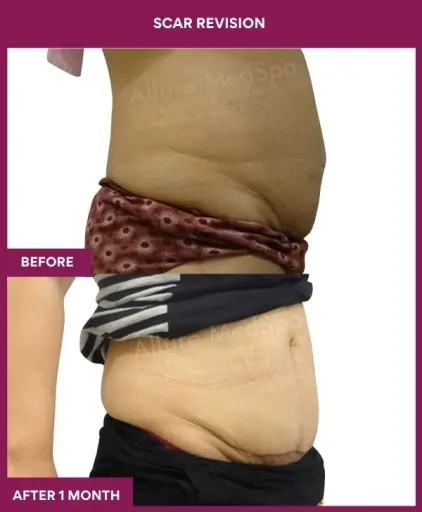
Scar Revision Surgery Before and After
“Liked the results? Let's plan yours.”
Scar Revision Surgery Testimonials: Fine To Fabulous Journeys
Awarded by Google.com
Rating: 4.7
Reviews: 485+
Awarded by WhatClinic.com
Rating: 4.8
Reviews: 119+
Awarded by Realself
Rating: 4.9
Reviews:453+
Awarded by Facebook
Rating: 4.6
Reviews:105+
Dr Milan Doshi and his staff are very professional and committed as the centre is highly equipped with advanced technology. I had closed rhinoplasty 4 months back and I’m seeing the results as to how it becomes successful.
Deepika Shetty
The doctor explained everything clearly and the surgery was smooth. Recovery was faster than I expected and the team was very supportive.
Rahul Mehta
Very natural results and excellent staff. From consultation to follow-up, the experience was outstanding and boosted my confidence.
Sneha Kapoor
“Inspired by their journey? Start yours”
- Do visible scars make you feel self-conscious, no matter how small they are?
- Are you reminded of past trauma or surgery every time you look in the mirror?
- Do you avoid certain clothes or social situations because of prominent marks on your face or body?
Scars aren’t just skin deep—they can impact your confidence, emotional wellbeing, and even limit your lifestyle. Whether they’re from burns, accidents, acne, or surgery, scars often carry a psychological weight that’s hard to ignore.
As a board-certified cosmetic surgeon with over two decades of experience, I’ve helped hundreds of patients achieve smoother, less noticeable skin through Scar Revision Surgery. This customized treatment improves the appearance of scars—making them finer, flatter, and better matched to your natural skin tone and texture—through medical-grade steroid therapy, laser resurfacing, or precision surgical techniques.
Global & Indian Trends: Scar Revision Surgery
- Scar revision remains one of the fastest-growing reconstructive aesthetic procedures worldwide.
- The ISAPS 2024 Survey reports a 13–14% global increase in scar-related treatments compared to the previous year.
- In India, high sun exposure and melanin-rich skin tones contribute to a strong demand for post-surgical and acne scar correction.
- At Allure Medspa, Mumbai, 900+ scar revision procedures have been performed with high patient satisfaction rates.
Source: ISAPS Global Survey 2024
Quick Facts for Scar Revision Surgery
| Time Required | 30mins to 2 Hours |
| Anesthesia | Local Anesthesia |
| Pain Level | Mild to Moderate Well Managed With Medications |
| Result | Final Result After 3 to 6 Months |
| Diet | No Restriction |
| Hospital Stay | Day Care Surgery |
| Flyback | 5-10 Days |
| Satisfaction Rate | More Than 95% |
| Complication Rate | Less than 1 to 2% |
| Hair Transplant Surgery Cost Mumbai, India | 15,000 to 50,000 INR |
Am I the Right Candidate for Acne Scar Treatment?
If you have stubborn acne marks affecting your confidence, there’s likely a safe, personalized solution—surgical or non-surgical—to improve your skin.
- Ice pick scars: May require punch excision or TCA CROSS technique
- Boxcar scars: Often treated with dermal fillers or fractional laser
- Rolling scars: Benefit from subcision or microneedling with RF
- Hyperpigmented marks: Managed with chemical peels or topical depigmenting agents
- Mixed scars: A combination approach delivers best results
Non-surgical treatments are often enough, but in some cases, advanced techniques like laser resurfacing or minor surgical revision are advised.
What Are Hypertrophic Scars and Their Best Treatment Options?
Hypertrophic scars are thick, red, raised marks that stay within the wound boundary. Steroid therapy and surgery help flatten and fade the scar.
- Frequently confused with keloids but less aggressive in growth.
- May fade naturally over time, especially with non-invasive treatment.
Treatment Options:
- Steroid creams or injections for early stage improvement.
- Surgical scar revision with repositioned incision lines.
- Intra-operative and post-operative steroid injections for prevention.
How Are Contracture Scars Caused and What Are the Treatment Options?
Contracture scars form after burns or major skin loss, restricting movement. Skin grafts, Z-plasty, and tissue expansion can restore flexibility.
- Caused by the skin tightening and pulling together during healing.
- Can impair muscles, tendons, and limit range of motion.
Treatment Options:
- Scar excision followed by skin graft or flap surgery.
- Z-plasty to release tension and improve mobility.
- Tissue expansion for extensive defects.
- Post-surgical physiotherapy often needed.
What Are Facial Scars and How Can They Be Improved Cosmetically?
Facial scars are often treated for cosmetic reasons using excision, dermabrasion, or repositioning techniques like Z-plasty for subtle blending.
- Due to visibility, facial scars cause aesthetic concerns.
Treatment Options:
- Precise excision and closure with fine sutures.
- Repositioning scars along natural skin creases (Z-plasty).
- Dermabrasion to blend scars into surrounding skin.
Results aim to make scars less noticeable, not fully erased.
What Are the Non-Surgical Options for Scar Improvement?
Non-surgical scar treatments like lasers, dermabrasion, microneedling, and steroid injections help reduce scar appearance with minimal downtime.
- Laser Therapy: Targets pigmentation, texture, and raised scars using fractional CO2 or pulsed dye lasers for smoother, more even-toned skin.
- Steroid Injections: Flatten and soften raised scars like keloids and hypertrophic scars by reducing inflammation and collagen buildup.
- Dermabrasion: Gently removes the top layers of skin using a high-speed rotating brush to improve surface-level scars and skin texture.
- Microneedling: Uses fine needles to stimulate collagen production and gradually improve pitted or atrophic scars with minimal invasiveness.
- Silicone Gel Sheets or Creams: Applied topically to hydrate and flatten scars over time—especially post-surgery or after injuries.
- Chemical Peels: Help improve superficial pigmentation or texture-related scarring through controlled exfoliation.
These non-surgical options are ideal for mild to moderate scars and can be used alone or combined for enhanced results. At Allure Medspa, Mumbai, we personalize your scar treatment plan based on skin type, scar depth, and your lifestyle preferences—with a focus on comfort, results, and minimal downtime.
What Are the Advanced Surgical Options for Scar Revision?
Advanced scar revision options include Z-plasty, skin grafts, and flap surgery—each tailored to improve function, reduce tension, and enhance aesthetics.
Z-Plasty:
A surgical technique that reorients scars along natural skin creases for better appearance and movement.
- Ideal for scars that cross relaxed skin lines or cause contracture.
- Involves excising the scar and repositioning triangular skin flaps into a “Z” shape.
- Performed under local anesthesia, typically as an outpatient procedure.
- Helps reduce scar visibility and relieves skin tension.
- Requires expertise in plastic surgery for best results.
Skin Grafting:
Transferring skin from a healthy donor site to a scarred or injured area.
- Commonly used for large wounds or deep scars.
- May result in scarring at both donor and recipient sites.
- Success depends on blood supply and graft “take.”
Flap Surgery:
Moves skin, fat, blood vessels, and sometimes muscle to the scarred area for improved function and aesthetics.
- Provides better texture, tone, and durability than grafts alone.
- Can be a pedicled flap (attached at one end) or free flap using microvascular surgery.
- Often preferred for complex or functionally limiting scars.
What Are the Pre-Operative Requirements for Scar Revision Surgery?
Before scar revision surgery, a few essential tests and instructions ensure you’re fully prepared for a safe and successful outcome.
Pre-operative steps help minimize risks and enhance results.
- Routine blood and urine tests
- Imaging (if needed based on scar depth or location)
- Discontinuing blood thinners and smoking before surgery
- Fasting for 6–8 hours (if undergoing surgical scar revision)
- Informing us about any ongoing medications or allergies
Your exact preparation may vary depending on the method used—laser, excision, grafting, or injectables. We’ll guide you through every step before the procedure.
What Is the Scar Revision Procedure and How Does It Improve Appearance?
Scar revision customizes treatments like lasers, steroids, or surgery to improve scar tone, texture, and blend—restoring confidence and skin harmony.
- Every scar is unique—caused by surgery, trauma, acne, burns, or injury.
- Treatment depends on scar type: keloid, hypertrophic, atrophic, contracture, or pigmented.
- Non-surgical options: steroid injections, laser therapy, dermabrasion, silicone sheets.
- Surgical options: excision, Z-plasty, skin grafting, flap surgery.
- Goal is to match scar with surrounding skin in tone, contour, and texture.
- Performed by Dr. Milan Doshi, board-certified cosmetic surgeon at Allure Medspa, Mumbai.
- Following pre- and post-care improves results and minimizes complications.
- Scar revision isn’t just cosmetic—it helps reclaim self-esteem and confidence.
What to Expect During Recovery After Scar Revision Surgery?
Recovery after scar revision involves wound care, mild restrictions, and avoiding sun exposure to support optimal healing and final results.
- Healing Time: Initial healing occurs within 1–2 weeks; full internal healing may take months depending on the technique used.
- Scar Care: Keep the area clean and dry, apply prescribed ointments, and follow all wound care instructions.
- Activity Restrictions: Avoid strenuous movements that may stretch or reopen the scar for at least 2–3 weeks.
- Stitch Removal: Usually done within 5–10 days, depending on scar location and depth.
- Sun Protection: Use SPF 50+ and cover the scar for at least 3–6 months to prevent darkening or pigmentation.
- Follow-Ups: Regular check-ins with your surgeon ensure healthy healing and reduce risks of complications.
How Soon Will You See the Final Results After Scar Revision?
Initial improvement is visible within weeks, but final results appear at 3–6 months as collagen remodeling and skin maturation take place.
- Early Results: Reduced redness, thickness, and smoother texture usually seen within 4–6 weeks.
- Collagen Remodeling: Your skin continues healing beneath the surface for up to 6 months post-procedure.
- Scar Fading: Pigment and texture gradually improve with time, especially with good sun protection and scar care.
- Enhancements: Some patients may benefit from follow-up treatments like lasers, microneedling, or steroid injections.
- Long-Term Outcome: Final appearance depends on skin quality, scar type, surgical technique, and post-op discipline.
What Are the Risks and Side Effects of Scar Revision Surgery?
Scar revision is generally safe, but risks may include pigmentation changes, infection, asymmetry, or scar recurrence in some cases.
- Hyperpigmentation: Sun exposure or healing issues can cause darkening of the revised scar.
- Recurrence: Keloids and hypertrophic scars can return, especially without compression or follow-up care.
- Infection: Rare but possible—managed with antibiotics and proper hygiene.
- Asymmetry: In very visible areas, slight irregularities in contour or position may occur.
- Wound Healing Delays: Smokers, diabetics, or those with poor immunity may heal more slowly.
- Allergic Reactions: To suture materials, dressings, or topical ointments (rare).
Choosing an experienced surgeon like Dr. Milan Doshi at Allure Medspa, Mumbai helps minimize these risks and ensures comprehensive aftercare.
How Much Does Scar Revision Surgery Cost in Mumbai, India?
Scar revision surgery in Mumbai typically costs between ₹15,000 to ₹50,000, depending on scar type, complexity, and surgical technique required.
Cost Range: ₹15,000 to ₹50,000 (approximate)
Key Cost Factors:
- Size and location of the scar
- Type of scar revision (single-stage or multi-stage)
- Need for tissue expanders or advanced techniques
What’s Included:
- Consultation with board-certified plastic surgeon
- Surgeon’s fees and anesthetist charges
- OT facility, consumables, and hospital stay
- Advanced technology and surgical equipment
- Immediate post-operative follow-ups
Not Included:
- Pre-operative fitness tests
- Post-op medications for home recovery
- Any rare or unforeseen health issues
Note: Cosmetic scar revision is not covered under insurance in India.
Expert Tip: Accurate pricing can only be given after a personalized consultation.
At Allure Medspa, Mumbai, we offer world-class scar revision treatments at affordable prices. Your consultation includes expert evaluation, solution planning, and full cost breakdown—no hidden surprises.
Want to know your personalized cost? Fill out the consultation form below or request a callback. Our counselor will reach out at your preferred time.
“Want to know the exact cost for you?”
Which Is the Best Cosmetic Treatment Centre for Scar Revision in Mumbai, India?
Allure Medspa, led by Dr. Milan Doshi, is Mumbai’s trusted centre for advanced scar revision with expert care, privacy, and natural-looking outcomes.
Why Choose Allure Medspa:
- Headed by renowned plastic surgeon Dr. Milan Doshi, known for natural-looking, precise results.
- Specialized in treating all types of scars—keloid, hypertrophic, atrophic, contracture, pigmented.
- State-of-the-art facility with advanced surgical and non-surgical scar revision options.
- Personalized care plans based on scar type, skin quality, and patient goals.
Types of Anesthesia Used:
- Z-plasty: Performed under local anesthesia, outpatient basis.
- Skin Grafting & Flap Surgery: Typically requires general anesthesia in hospital settings.
Rest & Recovery:
- Z-plasty stitches removed in a few days; fast recovery time.
- Grafts and flaps may need weeks or months to heal with support garments.
- Recovery success depends on strict adherence to post-op instructions.
Privacy & Comfort:
Allure Medspa follows the highest standards of patient privacy and confidentiality for your comfort and trust.
Post-Procedure Outlook:
- No scar can be erased completely, but expert techniques significantly improve appearance and texture.
- Final results depend on scar location, skin quality, healing response, and post-care discipline.
With the expertise of Dr. Milan Doshi and the cutting-edge infrastructure at Allure Medspa, your journey toward smoother, more confident skin begins with the right consultation. We don’t just revise scars—we restore self-image and confidence.
“Trust Mumbai’s leading aesthetic centre.”
Who Is the Best Cosmetic Surgeon for Scar Revision in Mumbai, India?
Dr. Milan Doshi is a board-certified cosmetic surgeon in Mumbai known for his expertise in scar revision, delivering natural-looking and precise outcomes.
- 30+ Years of Experience: Trusted name in aesthetic plastic surgery across India.
- Board-Certified: Certified by national and international cosmetic surgery associations.
- Specialization: Expert in treating all types of scars—keloid, hypertrophic, atrophic, contracture, and pigmented scars.
- Advanced Techniques: Offers cutting-edge treatments including Z-plasty, laser therapy, dermabrasion, skin grafting, and flap surgery.
- Thousands of Satisfied Patients: Renowned for delivering natural, confidence-restoring results.
- Personalized Care: Every treatment plan is tailored to your unique scar type, location, skin tone, and healing response.
- Allure Medspa, Mumbai: State-of-the-art facility focused on safety, precision, and privacy.
When it comes to life-changing procedures like scar revision, choosing the right surgeon matters. Dr. Milan Doshi’s surgical finesse and patient-first approach make him the most trusted cosmetic surgeon in Mumbai for achieving visible, lasting improvement in scar appearance.
“Ready to meet the expert?”
Medical Code for Scar Revision
ICD-10 Codes for Scar Revision Treatment
| ICD-10 Code | Description |
|---|---|
| L91.0 | Hypertrophic scar (raised, thickened scar tissue) |
| L91.8 | Other hypertrophic disorders of skin (keloids, thick scars) |
| L90.5 | Atrophic scar (sunken or depressed scars, e.g. acne) |
| T81.89XA | Other complications of procedures, initial encounter (for surgical scar complications) |
| Z41.1 | Encounter for cosmetic procedure (elective scar revision) |
CPT Codes for Scar Revision Treatment
| CPT Code | Description |
|---|---|
| 13120–13122 | Repair, complex, trunk/extremities/neck (for revision of wide/healed scars) |
| 13131–13133 | Repair, complex, forehead/cheeks/chin/mouth/nose/lips/eyelids (for facial scar revision) |
| 15780 | Dermabrasion, total face (commonly used for acne scar revision) |
| 15781 | Dermabrasion, localized area (e.g., single scar site) |
| 17110 | Destruction of benign skin lesions (for hypertrophic or keloid scars via laser/cautery) |
| 17999 | Unlisted procedure, skin (used for laser scar revision not otherwise specified) |
(FAQs) Frequently Asked Question for Scar Revision Surgery
Q1. Is scar revision surgery permanent?
Ans. Scar revision can significantly improve scar appearance, but no treatment can erase a scar completely. Results are often long-lasting, especially when post-care is followed.
Q2. Does scar revision look natural?
Ans. Yes, when performed by an experienced cosmetic surgeon, scar revision can make scars blend seamlessly with surrounding skin for a more natural look.
Q3. How painful is a scar revision?
Ans. Most scar revisions are performed under local anesthesia, so discomfort during the procedure is minimal. Mild soreness or tightness may be felt post-procedure.
Q4. What is the recovery time for scar revision?
Ans. Initial recovery takes 7–14 days, with full scar maturation occurring over several months. Downtime varies based on the technique and area treated.
Q5. Can laser treatments remove scars permanently?
Ans. Laser treatments can significantly fade scars and improve texture, but complete removal may not be possible. Maintenance sessions may be recommended for best results.
Q6. Can a dermatologist do scar revision?
Ans. Yes, board-certified dermatologists and cosmetic surgeons are trained in both non-surgical and surgical scar revision techniques, including lasers and excision.
Q7. Who is a candidate for scar revision surgery?
Ans. You may be a candidate if you have hypertrophic, keloid, contracture, or discolored scars that affect your appearance or function. Consultation is essential.
Q8. Can scar revision go wrong?
Ans. As with any procedure, risks exist—such as infection, pigmentation changes, or unsatisfactory cosmetic outcomes. Choosing an expert surgeon minimizes such risks.
Q9. What is the cost of scar revision?
Ans. The cost depends on the scar size, type, and technique used. It may range from ₹10,000 to ₹60,000 in Mumbai. Laser and surgical options vary in pricing.
Q10. What type of doctor does scar revision?
Ans. Cosmetic surgeons and dermatologists with expertise in scar management are the ideal specialists for scar revision procedures.
Q11. When is the best time to do scar revision?
Ans. Ideally, scars should be treated after they’ve matured—typically 6–12 months after injury. However, early intervention may be considered in specific cases.
Q12. Do you need anesthesia for scar revision?
Ans. Most procedures are performed under local anesthesia. Larger revisions may require sedation or general anesthesia depending on complexity.
Q13. What are the disadvantages of scar revision?
Ans. Risks include incomplete improvement, pigmentation issues, recurrence in keloids, or rare complications like infection or poor healing.
Q14. Can insurance cover scar revision surgery?
Ans. Cosmetic scar revisions are typically not covered. However, reconstructive procedures following trauma or burns may be partially reimbursable.
Q15. Is laser scar removal painful?
Ans. Laser treatments feel like mild snapping or heat on the skin. A numbing cream is usually applied beforehand to ensure comfort.
Q16. Can scar revision be done on the face?
Ans. Yes, facial scar revision is common and performed with precision using lasers, microneedling, or minor surgery to ensure minimal visibility.
Q17. What are the problems with scar revision?
Ans. Challenges may include unpredictable healing, skin sensitivity, or dissatisfaction with results. These are minimized with realistic expectations and expert care.
Q18. How to remove scars from the face permanently?
Ans. While permanent removal isn’t guaranteed, treatments like fractional lasers, microneedling, and excision can significantly fade facial scars over time.
Q19. Is scar revision free?
Ans. No, scar revision is a specialized cosmetic procedure and is usually chargeable unless medically necessary under insurance coverage.
Q20. How long is recovery from scar revision?
Ans. Initial healing takes 1–2 weeks, but full results may appear in 3–6 months as the skin remodels. Gentle care and sun protection are essential post-treatment.
“Still have questions? We’re here.”
Related Links
Note: The author of this content is Dr. Milan Doshi, An Indian board-certified plastic & cosmetic Surgeon wholly & solely confirms the authenticity of the information & knowledge delivered by this write-up.